Know What are the Symptoms of Plantar Fasciitis
Before we go further and discuss the symptoms of plantar fasciitis, it is important to understand what plantar fasciitis is and what causes it. Today we are going to cover all these aspects for a better understanding of the subject.
Definition:
Plantar fasciitis (pronounced “plantar fash-eee-eye-tiss”) literally means “inflammation of the plantar fascia.” Plantar fasciitis is also known as “Policeman’s Heel”. Plantar fasciitis is often associated with heel spurs (heel spurs). The plantar fascia is a ligament that connects the heel to the front of your foot. It’s thick and web-like and acts like a shock absorber, so you won’t have any problems walking, running and even jogging.
Plantar fasciitis is one of the most common diseases of the heel. Like the other parts of our body, the plantar fascia also undergoes a lot of wear and tear. In fact, it undergoes many extreme situations on a daily basis. Too much pressure tends to take its toll on the feet and the ligaments tend to tear. As a result, the plantar fascia becomes inflamed and red, which in turn leads to stiffness and pain in the heels. While the exact cause of this disease is not certain, we cannot deny that we need to rest our feet if we want to stay healthy. Remember that your feet bear the entire weight of your body. What Are the Common Symptoms of Plantar Fasciitis?
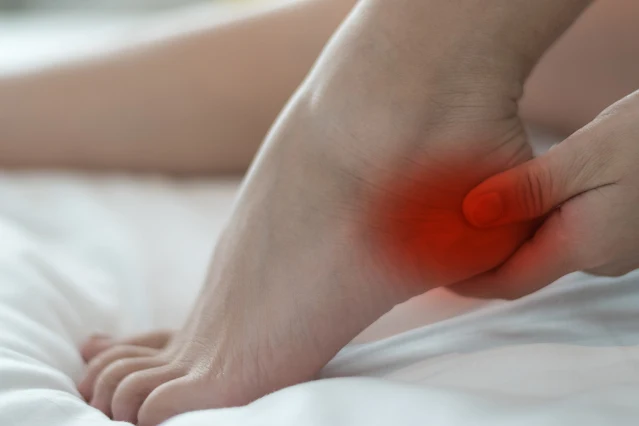
- One of the most common symptoms is pain at the bottom of the heel. Sometimes this pain is also felt in the middle of the foot. It generally affects one foot, but it can also affect both feet.
- The intensity of the pain increases with the passage of time. The pain may be sharp like needles or dull like a thud. Many experience a burning sensation on the bottom of the foot that extends outward from the heel.
- The pain is often severe in the morning when you get up from your sleep and try to take the first steps out of bed. You will experience a sharp pain if you have been sitting still for too long or simply lying down for too long. If you have stiffness in the heel, you will experience pain when you try to climb the stairs.
- The pain tends to increase after any prolonged activity. This is because inflammation has increased and irritation has increased. If you suffer from plantar fasciitis you will not experience any pain during the activity. The pain starts to register as soon as you stop the activity.
Anatomy:
The plantar fascia is a thick, fibrous band of connective tissue that runs like a fan from the heel bone (calcaneus) along the sole of the foot and is attached at the other end to the base of each of the toes. It is a tough and resilient ligament structure that performs a crucial function during walking and running.
The Plantar Fascia acts as a ‘bowstring’ connecting the ball of the foot to the heel. It forms the longitudinal arch of the foot and helps lift the heel off the ground to prepare the foot for the ‘start’ (propulsive) phase of the gait cycle. When walking, the moment the heel begins to lift off the ground, the plantar fascia endures a tension roughly double our body weight. The Plantar Fascia also acts as a natural shock absorber when walking and running.
Read also about Pregnancy Pillow | Christmas Decoration | T20 world cup live stream free
Causes Of Plantar Fasciitis:
Plantar fasciitis is Latin for inflammation of the plantar fascia. This inflammation occurs at the point where the fascia attaches to the calcaneus (also known as the heel bone).
So what causes the plantar fascia to become inflamed? There are a number of different reasons why this happens. For example, you are more likely to develop plantar fasciitis if you are over 50 years old, if you are overweight, or pregnant, or if you have a job that involves a lot of walking or standing on hard surfaces. You are also at risk if you walk or run a lot for sports (overuse injuries). And if you have tight calf muscles (which many people have), you’re also more likely to develop plantar fasciitis.
However, research has shown that the No. 1 cause of plantar fasciitis is overpronation (or fallen arches).
Overpronation of the feet is very common, at least half of the population has this problem, but most people don’t realize they have this condition! Overpronation simply means that the feet and ankles roll in too much when walking and that the arches collapse. With age, most people tend to overpronate. However, this condition is not uncommon in children and teenagers, as well as athletes.
When the arch collapses, the two outermost points of the arch (the heel and ball of the foot) are moved further apart. This puts repeated stress on the plantar fascia. The attachment of the fascia in the heel bone is a small area of tissue, compared to the broad attachment area at the toes. Therefore, the constant excessive pulling on the fascia will damage the weakest attachment point.
Over time, irritation occurs at the heel bone, followed by inflammation and micro-rupture of the plantar fascia tissue. Sometimes there is swelling. As the pull continues, the heel bone will ‘react’ and a bony growth develops at the front of the heel bone. This is called a ‘heel spur’. Interestingly, the heel spur itself does not cause pain, but the inflamed tissue around it does.
Do you suffer from any of the common symptoms of plantar fasciitis? If so, you must make an appointment with the orthopedist at the earliest. Have yourself checked thoroughly. If the doctors ask you to have an X-ray and other tests, get it done as soon as possible. It is important to get yourself treated. Ignoring the heel pain will be the biggest mistake of your life. Soon you will have a limp and then you will be dependent on crutches for the best of your life.
Ask your friends and family if they can recommend a good orthopedist. You can also search online. Find out who is the leading orthopedics in your city. Call them one by one to see who is currently available and book your appointment at the earliest. When you go to the doctor, explain to him in detail what you are experiencing. There is nothing to be ashamed of. In fact, if you don’t have any questions about the treatment, ask them too. Clarify all your doubts from the start.
Plantar Fasciitis Treatment Options:
Fortunately, most cases of plantar fasciitis can be treated well at home. First, you should refrain from activities that cause pain, such as long walks, running, exercising, and standing for long periods. Rest ensures that any swelling, inflammation and/or pain disappear.
Applying ice (or a heat pack) to the heel and using anti-inflammatory pain relievers such as Advil or Nurofen (both contain ibuprofen) will provide immediate pain relief.
However, an effective long-term treatment for plantar fasciitis consists of a simple program of daily stretching exercises, combined with wearing an orthosis to support the arches.
Gently stretching the plantar fascia, Achilles tendon, and calf muscles will make your feet and feet more flexible, which in turn will help reduce over-pulling of the plantar fascia. Do the stretches first thing in the morning and avoid walking barefoot on hard floors and tiles. Instead, put on a pair of shoes with an orthosis in them. Repeat the exercises (especially the calf stretches) a few times throughout the day.
The complete Plantar Fasciitis stretching program can be found here. Or talk to your physical therapist or podiatrist about specific exercises. Sometimes practitioners will prescribe a night splint designed to gently stretch the fascia at night.
With the combination of daily exercises and orthoses you will see a big improvement within a few weeks. If you are overweight, it is advisable to lose some weight as it will reduce the strain on your feet.
In cases where the pain is persistent or severe, plantar fasciitis can be treated with a cortisone steroid injection into the heel. However, this is only a short-term solution and the pain will return within 3 months. A newer treatment for plantar fasciitis (set up prior to surgery) is electrocorporeal shock wave therapy. In this procedure, an instrument delivers pulses of energy (shock waves) to your heel to relieve pain.
Surgery for plantar fasciitis is rarely necessary unless all other treatments have failed to relieve the pain. Surgical procedures involve removing part of the plantar fascia.
Plantar Fasciitis and Orthotics:
Research in America, Europe and Australia has clearly shown that wearing an orthotic insole is the best way to treat plantar fasciitis, especially when combined with daily exercise. However, it should be noted that this treatment regimen is especially effective for people who helped recently (i.e. no more than 6-8 weeks ago) or for those who only experience mild plantar fasciitis pain.
The reason why an orthosis works is simple: the cause of plantar fasciitis is the constant pulling of the “arch tendon” under the foot, due to the sagging of the arches. Orthotics prop the arches back up, reducing the undue stress on the plantar fascia.
With less stress on the plantar fascia, the damage to the ligament can be reversed. The tissue is allowed to heal faster and repair the micro-tear that occurred at the heel bone attachment.
There are different types of orthoses, also custom made by a podiatrist. However, not everyone needs a custom device. Today, good supportive and inexpensive orthotics are available from retailers and specialist websites. The most important factor is support, more than cushioning. So don’t buy a soft, spongy or gel footbed, but an insole with a high arch, made of fairly sturdy materials.
Tips To Prevent Plantar Fasciitis:
Correcting some of the predisposing factors will ensure that plantar fasciitis does not recur, for example:
1. Maintain a Healthy Weight: Lose some weight as it reduces the physical strain on the plantar fascia when walking
2. wear good quality supportive shoes: i.e. shoes with a strong heel counter and good flexibility at the front of the shoe (allowing the toes to bend back easily and naturally). A good shoe helps stabilize the heel and ankle joints when walking and running.
Do not wear completely flat shoes. An elevated heel reduces tension in the plantar fascia.
3. try to avoid walking barefoot on hard surfaces (including hard sand on the beach)
4. Always stretch your calf muscles before exercising (walking, running or exercising). Greater flexibility in the tissue makes them less prone to damage.
Thanks for Reading about What are the Symptoms of Plantar Fasciitis
Visit our Facefook Page
Keywords: What are the Symptoms of Plantar Fasciitis